Minor Operative or Minor Operative Procedures
With the long hospital waiting lists, which have been exacerbated by the pandemic, both for consultations and then the procedures, we aim to see the patients for consultation promptly in 1-2 weeks and aim to either perform the procedure on the same day if the patient is suitable for the procedure and wishes to proceed or aim to perform the procedure for suitable patients within 1-3 weeks following consultation.
Alongside our range of Aesthetic medical procedures, we offer non aesthetic minor surgical procedures at Excellence Medical. The minor operative procedure list below is not exhaustive and we can other procedures not mentioned in the list below.
Please visit our other websites :
https://circumcisionclinic.ie
The most common minor operative procedures performed under local anesthesia are as follows :
Skin tags Removal – These benign skin growths that project over the skin from a relatively small, narrow stalk. They are commonly found on the eyelids, under the breasts, on the neck and underarms. They can be irritating and frequently get inflammed due to friction with the clothing or jewellery. Also, they can be cosmetically bothersome. We remove these skin tags simply under local anaesthesia and send them for histological examination.
Moles Removal – We go through the medical history and make a physical assessment of moles to access that it may not be malignant. They are easily removed with little if any side effects under local anaesthetic. Sutures may be required for a few days and some scarring may follow removal. This, however, will reduce and become less noticeable over time. We send the excised samples for histological examination.
Sebaceous cysts Removal – Sebaceous cysts may be found on the Scalp, trunk, face, neck and other parts of the body. They are caused by blockade of oil(sebacous) secreting glands, and take the form of a globular lump under the skin. Generally, they are benign painless lumps under the skin, but have a potential to become infected and gradullay becoming larger over time. This is best avoided by removal under local anesthesia. Cysts are either removed under local anaesthesia. They may need incision/drainage through an incision if they are infected and contain pus. The specimen is sent away for histological examination.
Lipoma Removal – Lipomas are benign fatty lumps and are movable rounded lumps under the skin. Lipomas range in size and sometimes can be quite deep and large in size, termed ‘giant lipomas’. They are usually slow-growing lumps in the subcutaneous tissue, beneath the skin. There removal is a simple procedure, performed under local anaesthesia. The lipoma specimen is sent for histological examination.
Ganglion Cyst Treatment– These are globular sac-like lumps or cysts that are formed from internal degeneration of a tendon. They are often found on the wrist and ankle on the long extensor tendons. Ganglion cysts are aspirated and injected with a steroid medicine under local anesthesia.
Scar revision – Scar revision is surgery to improve the cosmetic appearance of scars. It also restores function and corrects skin disfigurement. Scars are caused by an injury wound which can be due to variety of causes including previous surgery. We assess each scar on its individual merit and will discuss the most appropriate treatment suitable which may range from scar revision, to steroid injection etc.
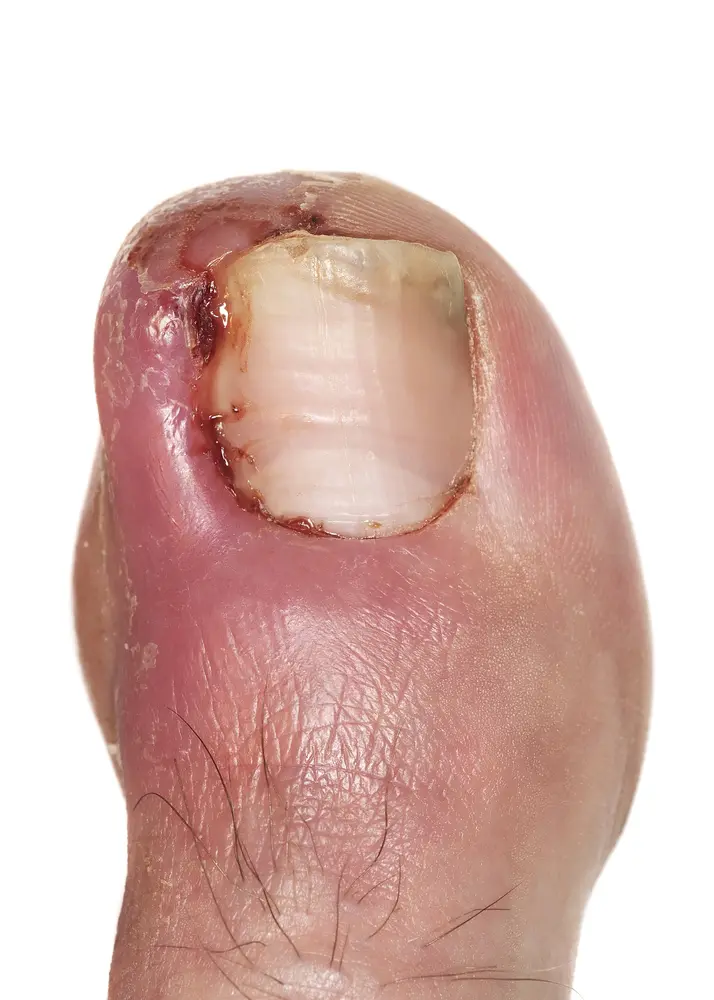
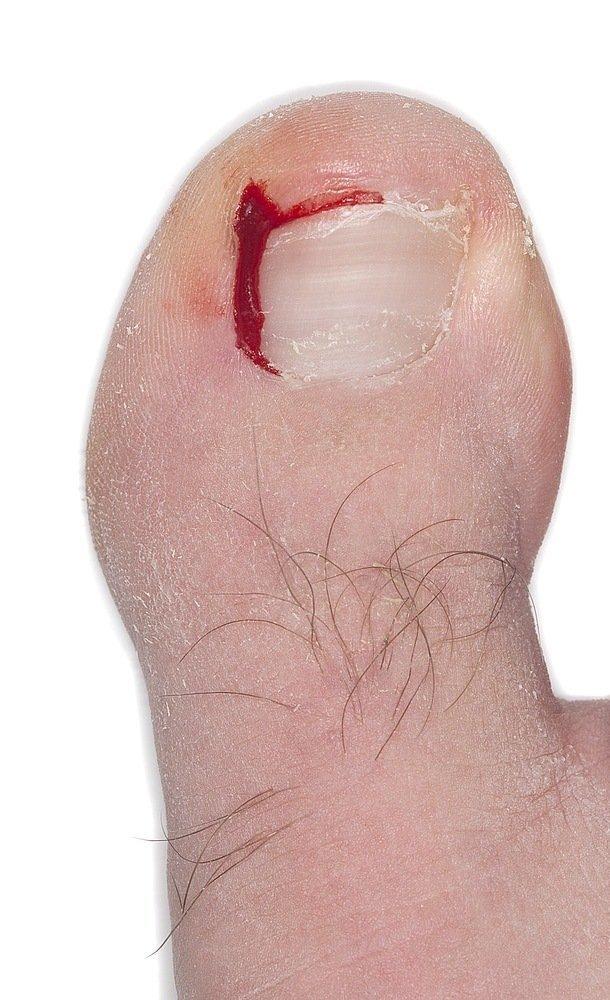
Ingrowing Toe Nail Surgery : An ingrown toenail develops when the sides of the toenail grow into the surrounding skin and pierces it causing inflammation. The big toe is often affected, either on one or both sides. The nail curls and pierces the skin, which becomes painful, red, swollen and tender.
Before your Minor Surgery
1.You are advised to have a light meal before arrival to the clinic. There is no requirement to fast for a procedure performed under local anesthesia.
2. It is usually best to arrange for somebody else to take you home after your minor operation. Although it’s very unlikely to be a problem, we do not advise driving or travelling unaccompanied by public transport in case you feel unwell.
3.It helps to wear loose fitting clothing. We usually only need to expose the affected part to be operated upon.
4.We pride ourselves on making the procedure and post procedure recovery period as pain free and comfortable as possible.
5.You will be awake throughout the procedure and no intravenous sedation is given.
6.You will be given local anaesthesia with a very fine needle injection to make the operative area go numb. You will feel mild discomfort for a few seconds as the anaesthetic is administered. Thereafter, you will feel no pain.
7.Apart from a parent accompanying a young child, we are not able to accommodate companions in the minor surgery room but they are welcome to sit in the waiting room whilst you are having your minor operation.
Aftercare of your Minor Surgery
1. You should take it easy and rest for the remainder of the day after your minor operation.
2. Unless advised otherwise, wound dressings should be kept dry and intact for 24 to 48 hours or as advised. After 24 to 48 hours you may have a shower. Do not use bubble bath or talcum powder for about 10 days as it could irritate the wound and impair the healing process. It can also predispose the wound to an infection.
3. Not all minor operative procedures involve sutures. If you have non-dissolving stitches, you will need to book an appointment to have your stitches removed. The duration of the sutures will be advised after the minor operation. We recommend that you book this appointment on the day of your minor operation before you leave. As a general rule, sutures to the head and neck area are removed at 5-7 days after your operation and other parts of the body may have stitches removed between 10-14 days. Mr.Roy will advise you of exactly when your stitches should be removed before you leave.
4. The local anaesthetic used ( lignocaine) usually lasts for 4 hours following administration. We recommend that you start to take your painkillers as advised after your operation so that you are as comfortable as possible in the post operative recovery period.
5. Suitable over the counter painkillers are paracetamol or ibuprofen.
6. Incidence of wound infection is usually less then 1%. Signs of infection include fever, increasing redness around the wound and a mucky yellow discharge. In the unlikely event that you are concerned that you may have developed an infection, please contact us.
7. You should be able to return to normal activities, as soon as you feel able.
8. Most patients will be back at work the next day.
9. Please avoid heavy exercising and swimming for 2 weeks.
Ingrown toenail / Ingrowing toenail
Overview
An ingrown toenail develops when the sides of the toenail grow into the surrounding skin and pierces it causing inflammation.
The big toe is often affected, either on one or both sides. The nail curls and pierces the skin, which becomes painful, red, swollen and tender.
Common symptoms include:
- pain if pressure is placed on the toe
- inflammation of the skin at the end of the toe
- a build-up of fluid (oedema) in the area surrounding the toe
- an overgrowth of skin around the affected toe (hypertrophy)
- bleeding
- white or yellow pus coming from the affected area
What causes ingrown toenails?
The following can contribute in causing an ingrown toenail to develop :
- badly cut toenails – cutting your toenails too short, or cutting the edges, will encourage the skin to fold over your nail and the nail to grow into the skin
- wearing tight-fitting shoes, socks or tights – this places pressure on the skin around your toenail; the skin may be pierced if it’s pressed on to your toenail
- sweaty feet – if the skin around your toenails is soft, it’s easier for your nail to pierce it and embed itself within it
- injury – for example, stubbing your toe can sometimes cause an ingrown toenail to develop
- natural shape of the nail – the sides of curved or fan-shaped toenails are more likely to press into the skin surrounding the nail
Treatment for ingrown toenail :
Left untreated, an ingrown toenail can become infected, so it’s important that you:
- keep your feet clean by washing them regularly and keeping them clean and dry.
- change your socks regularly
- cut your toenails straight across to stop them digging into the surrounding skin
- gently push the skin away from the nail using a cotton bud (this may be easier after using a small amount of olive oil to soften the skin)
- wear comfortable shoes that fit properly
Surgery may be recommended if your toenail doesn’t improve. Depending on the severity of your symptoms, this may involve removing part or all of your toenail.
1. Partial nail avulsion
Partial nail avulsion removes part of your toenail under local anaesthesia and is the most commonly used operation for treating ingrown toenails.
A local anaesthetic medicine is used to numb your toe and the ingrown part of your toenail is cut away. Any pus is drained and dead tissue is debrided.
A course of an antibiotic may be prescribed if your nail is infected.
2. Total nail avulsion
Total nail avulsion completely removes your toenail. This may be necessary if your nail is thick and pressing into the skin surrounding your toe on both inner and outer sides in the same toe.
After surgery
After toenail surgery, your toe will be wrapped in a sterile bandage. This will help prevent any bleeding and also prevent infection. Rest your foot and keep it raised for 1 to 2 days after the operation.
To help reduce the pain, you may prescribed a pain killer. Wear soft or open-toed shoes for the first few days after surgery.
Preventing ingrown toenails
Taking care of your feet will help prevent foot problems such as ingrown toenails. It’s important to cut your toenails properly (straight across, not at an angle or down the edges).
Wash your feet every day, dry them thoroughly and use foot moisturiser.
Wearing shoes that fit properly will help to ensure your feet remain healthy. You should also change your socks (or tights) every day.
Joint Injection Treatments for Osteoarthritis
Joint injections or aspirations (taking fluid out of a joint) are performed often with local anaesthesia. After the skin surface is thoroughly cleaned, a needle in injected directly into a joint. At this point, either joint fluid can be removed (aspirated) and used for appropriate laboratory testing. Steroids, Platelet Rich Plasma (PRP) or adipose ( fat ) derived Stem Cells can be injected into the joint according the indication of treatment. These treatments can treat inflammation inside the joint, leading to decreased swelling and pain with to effective pain management and in turn translate into a better quality of life.
Commonly injected joints include the knee, Hip joint, shoulder, ankle, elbow, wrist, base of the thumb, and small joints of the hands and feet.
- Joint injections are used to deliver the therapeutic agent directly into a joint, such as a knee, ankle, or wrist. Sometimes fluid is removed from the joint before the steroid is injected.
- Steroid joint injections can help with pain and swelling by treating the underlying joint inflammation – improvement is often quick.
- The risks for joint aspirations and injections are minimal. Infection, bleeding, and other risks are rare.
What is a joint aspiration or joint injection?
Steroid joint injections can be used as part of a treatment plan for people with arthritis. A medication/PRP/Stem Cells is injected using a needle directly into a joint, such as a knee. The steroid treats the inflammation inside the joint, leading to decreased swelling and pain.
Sometimes joint fluid is removed before the steroid is injected (called aspiration), and then the therapeutic agent is injected into the joint, without requiring a new needle stick. Fluid obtained from a joint aspiration can be examined by the physician or sent for laboratory analysis, which may include a cell count (the number of white or red blood cells), crystal analysis (to confirm the presence of gout or calcium pyrophosphate crystal disease), and/or culture (to determine if an infection is present inside the joint). Drainage of a large joint effusion can provide pain relief and improved mobility.
The decision to use joint injections as part of a treatment depends on each individual case. Joint injections may decrease the accumulation of fluid and cells in the joint and may decrease pain and stiffness. The positive effects of joint injections are for pain management and better quality of life and may not be permanent. Often, the improvement in inflammation, swelling and joint pain lasts a long time before needing another treatment, but depends on the extent of the joint osteoarthritis. In some milder conditions, a joint injection may produce long periods of disease control.
Steroid joint injections may be given to treat inflammatory joint conditions, such as rheumatoid arthritis, psoriatic arthritis, gout, tendonitis, bursitis and, osteoarthritis.
How is a Joint Injection usually given?
Joint injections can be performed safely in the clinic. It is important for the patient to stay still during the procedure. Hyaluronic acids and corticosteroids (such as methylprednisolone and triamcinolone formulated to stay primarily in the joint) are frequently used. Corticosteroids are anti-inflammatory agents that slow down the accumulation of cells causing inflammation and pain within the joint space.
When it is time for the injection, the skin at and around the injection site will be carefully cleaned to remove bacteria from the skin. A needle is then inserted into the joint space. If the plan is to remove fluid, an empty syringe will be attached to the needle to pull the fluid out. Sometimes, multiple syringes need to be used to remove all the fluid. After any necessary fluid is removed, a small syringe containing the therapeutic agent is attached to the needle and is slowly injected into the joint. The needle is removed, and pressure is held to prevent any bleeding. A bandage is applied to the injection site.
Possible Risks/Side Effects
Infections are very rare complications of joint injections. Another uncommon complication is post-injection flare – joint swelling and pain several hours after the injection – which occurs in approximately 1 out of 50 patients and usually subsides within several days. Some patients may have a temporary increase in pain that can last a few days and is usually manageable with pain killer medication,
Other complications, which is associated with a corticosteroid injection treatment may include depigmentation (a whitening of the skin), local fat atrophy (thinning of the skin) at the injection site and rupture of a tendon near the injection site.
Joint injections also should not be given if an infection is present inside or around a joint and if someone has a serious allergy to one or more of the medications that are injected into a joint. If an infection is suspected, aspirating the joint to gather cultures is essential.
Request Consultation

- Pilar Cysts - 8th Feb 2022
- Pilonidal Cyst and Pilonidal Sinus - 6th Feb 2022
- Sebaceous Cyst - 7th Apr 2020
